Introduction
Rheumatoid arthritis (RA) is a chronic autoimmune disease that affects the joints and other parts of the body. It can cause pain, stiffness, and swelling in the joints, as well as fatigue and other symptoms.
Early diagnosis and treatment are important for managing RA and preventing further joint damage. If you’re wondering whether you might have RA, there are several signs and symptoms to watch for. In this article, we’ll cover how do I know if I have rheumatoid arthritis and what you need to know about RA, and how to determine if I might have it.
What is Rheumatoid Arthritis?
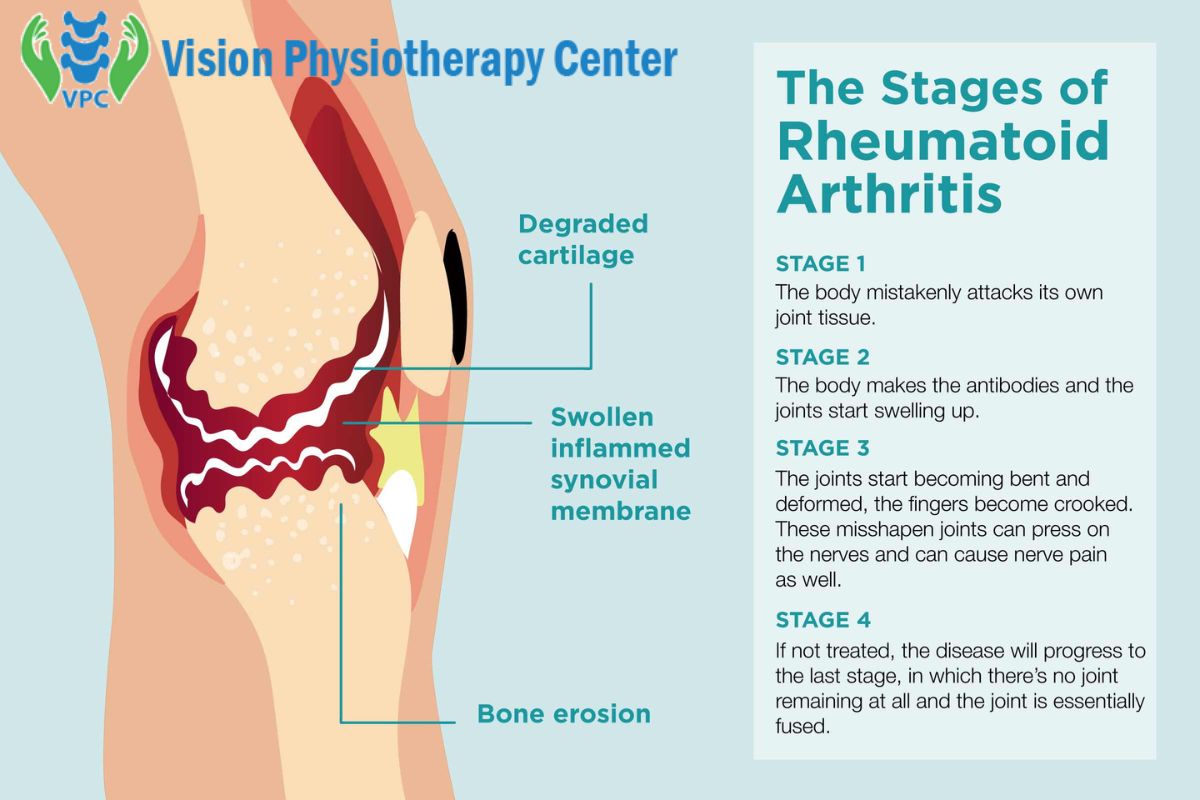
Rheumatoid arthritis is an autoimmune disorder that affects the joints, causing pain, swelling, stiffness, and eventually, loss of function. In this condition, the immune system mistakes healthy cells and tissues for foreign invaders and attacks them, resulting in inflammation of the joints.
This chronic inflammation can lead to cartilage and bone damage, and as the disease progresses, it can affect other organs and systems in the body. It typically affects the smaller joints in the hands and feet first but can occur in any joint. Women are more likely to develop rheumatoid arthritis than men, and the condition usually begins in middle age, although it can occur at any age.
While there is no cure for rheumatoid arthritis, treatments such as medications, physical therapy, and lifestyle changes can help manage symptoms and slow the progression of the disease, improving the quality of life for those who are living with it. Individuals with RA need to work with a physiotherapist to develop a treatment plan that meets their specific needs and goals.
Causes of Rheumatoid Arthritis
Understanding the Root of the Problem. Rheumatoid arthritis (RA) is a chronic autoimmune disease that affects millions of people worldwide. It is a painful condition that can lead to disability if left untreated. The exact causes of RA are not yet fully understood, but research suggests that several factors may contribute to its development.
- Genetics: Some people may have a genetic predisposition to developing rheumatoid arthritis. Studies have found that certain genes can increase the likelihood of developing the condition.
- Environmental factors: Exposure to certain environmental factors, such as smoking or air pollution, may increase the risk of developing rheumatoid arthritis.
- Hormonal factors: Rheumatoid arthritis is more common in women than in men, leading some experts to believe that hormonal factors may play a role in the development of the disease.
- Immune system dysfunction: Rheumatoid arthritis is an autoimmune disease, meaning that the immune system attacks healthy cells in the body. It is thought that a malfunctioning immune system may be a key factor in the development of the disease.
- Infections: Some researchers believe that infections, such as those caused by viruses or bacteria, may trigger the development of rheumatoid arthritis in susceptible individuals.
- Lifestyle factors: Obesity and a sedentary lifestyle have been associated with an increased risk of developing rheumatoid arthritis.
It’s important to note that the exact causes of rheumatoid arthritis are still not fully understood and that the disease is likely caused by a combination of genetic, environmental, and lifestyle factors.
What are the Five Signs of Rheumatoid Arthritis?
Here are five signs and symptoms of rheumatoid arthritis:
- Joint Pain and Stiffness: RA can cause pain, swelling, and stiffness in the joints. The pain is usually worse in the morning or after periods of inactivity.
- Joint Redness and Warmth: Inflammation in the joints can cause redness and warmth around the affected area.
- Fatigue: Many people with RA experience fatigue, which can be caused by inflammation in the body and the stress of dealing with chronic pain.
- Loss of Range of Motion: RA can cause a loss of range of motion in the affected joints, making it difficult to move them as freely as before.
- Joint Deformity: Over time, RA can cause joint damage and deformity, especially if left untreated. This can affect a person’s ability to perform daily tasks and lead to disability.
Understanding Rheumatoid Arthritis
Before we dive into the symptoms of RA, it’s helpful to understand what it is and how it differs from other types of arthritis. RA is an autoimmune disease, which means that the immune system attacks healthy tissues in the body, causing inflammation and damage. how do I know if I have rheumatoid arthritis?
In the case of RA, the joints are the primary target of this autoimmune response. This can lead to chronic inflammation in the joints, as well as damage to other parts of the body, such as the lungs, heart, and eyes.
Unlike osteoarthritis (OA), which is a degenerative joint disease caused by wear and tear on the joints over time, RA can affect people of any age and tends to progress more rapidly.
RA also tends to affect multiple joints simultaneously, rather than just one or two as with OA. In addition, RA symptoms may come and go, with periods of flare-ups followed by periods of remission.
Signs and Symptoms of Rheumatoid Arthritis
So, how do I know if I have rheumatoid arthritis?
Here are some of the most common signs and symptoms to watch for:
Joint Pain and Stiffness
One of the hallmark symptoms of RA is joint pain and stiffness, especially in the morning or after periods of inactivity. This pain and stiffness may affect multiple joints, such as the hands, wrists, feet, and knees. The pain may also be accompanied by swelling and redness in the affected joints.
Fatigue
Many people with RA experience fatigue, even if they’re getting enough sleep. This can be due to the body’s immune response, as well as the physical strain of dealing with chronic pain and inflammation.
Weakness
RA can also cause weakness and muscle wasting, especially in the hands and feet. This can make it difficult to grip objects or perform daily tasks.
Joint Deformities
Over time, RA can cause joint deformities, especially in the hands and feet. This can include nodules or bumps on the joints, as well as changes in the shape of the joints themselves.
Eye Problems
RA can also cause eye inflammation, leading to dryness, redness, and sensitivity to light. In rare cases, it can also cause more serious eye conditions, such as scleritis or uveitis.
Lung Problems
RA can also affect the lungs, causing inflammation and scarring that can make it difficult to breathe. This can lead to conditions such as interstitial lung disease or pulmonary hypertension.
Diagnosis and Rheumatoid Arthritis Treatment
Diagnosis of rheumatoid arthritis (RA) typically involves a combination of medical history, physical exam, blood tests, and imaging studies. Once a diagnosis has been made, treatment usually involves a combination of medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), disease-modifying antirheumatic drugs (DMARDs), and biologics.
In addition, physiotherapy can be an important part of managing RA. A physiotherapist can help you develop an exercise program that can improve your range of motion, strengthen your muscles, and reduce your pain and stiffness.
They can also teach you techniques for protecting your joints and conserving your energy, as well as provide other forms of therapy, such as cryotherapy and pulse electromagnetic therapy. Working with a physiotherapist can help you better manage your RA and improve your overall quality of life.
Final Thought
Rheumatoid Arthritis (RA) can be a challenging and often debilitating condition, but with early diagnosis and appropriate treatment, it is possible to manage the symptoms and maintain a good quality of life. In this blog post, we have discussed, how do I know if I have rheumatoid arthritis.
It’s important to work closely with your rehabilitation team to develop a personalized treatment plan that addresses your unique needs and goals. Additionally, lifestyle modifications, such as maintaining a healthy diet and exercise routine, can also play a crucial role in managing RA. With the right support and care, those living with RA can lead fulfilling lives and continue to pursue their passions and interests.
Written by.
Dr. Saiful Islam, PT
BPTh (DU), MPTh (Orthopedics) – NIPS, India
PG Certificate in Acupuncture, India
Specially trained in Ozone Therapy, USA and Ozone Forum, India.
Physiotherapy Consultant, Vision Physiotherapy Center.
To consult: 01760-636324 , 01932-797229 (9:00 AM to 9:00 PM) and make an appointment.
Our Facebook page: Vision Physiotherapy Center